Understanding Psoriasis Flare Symptoms Effectively


Intro
Psoriasis is a chronic autoimmune condition that manifests on the skin. It is known for its unpredictable flare-ups, which can lead to significant physical and psychological discomfort. Understanding psoriasis flare symptoms is crucial for effective management and improved quality of life. This guide aims to unpack the various symptoms, triggers, and management strategies associated with psoriasis, providing valuable insights into the condition.
Article Overview
Summary of Key Findings
Psoriasis is more than skin deep. Research highlights that flare symptoms can vary widely among individuals. Common symptoms include red patches, silvery scales, and itching, which can be aggravated by many factors. Notably, the impact of psychological stress on psoriasis is recognized in recent studies, illustrating a complex interplay between mental and physical health.
Research Objectives
The primary goal of this article is to elucidate the symptoms of psoriasis flare-ups, their associated triggers, and best practices for management. By doing so, the piece aims to empower individuals with psoriasis, along with caregivers and healthcare providers, to navigate the complex landscape of this condition more effectively.
Key Results and Discussions
Main Findings
- Symptom Variability: Psoriasis symptoms can differ in severity and presentation. Factors such as age, genetics, and environmental influences can affect individual experiences.
- Triggers Identified: Common triggers for flare-ups include stress, infections, certain medications, and skin injuries. Recognizing these can aid in prevention strategies.
- Psychological Impact: The burden of psoriasis extends beyond the skin. Individuals may experience anxiety, depression, and low self-esteem due to their condition. Acknowledging this aspect is important for holistic care.
Implications of Findings
The findings suggest a need for personalized treatment approaches. Healthcare providers must assess each patient's unique symptomatology and triggers. Furthermore, understanding the psychological component can lead to additional therapeutic interventions that address mental health, making a significant difference in the lives of those affected by psoriasis.
"Understanding the multifaceted nature of psoriasis provides a more comprehensive treatment approach, addressing both the physical and mental aspects of the condition."
By highlighting these elements, the guide aims not only to inform but also to create a pathway toward better management and support for individuals living with psoriasis.
Prelims to Psoriasis
Psoriasis is more than a mere skin condition; it is a chronic autoimmune disorder that can impose significant physical and emotional challenges on those affected. Understanding psoriasis is crucial for comprehending the flare symptoms that stem from this ailment. The condition manifests through an abnormal immune response that accelerates skin cell production. This leads to the characteristic plaques found on the skin's surface.
Both the physiological and psychological dimensions of psoriasis deserve attention. It is essential to recognize that physical symptoms, like itchy patches and red lesions, are not the only concerns. The emotional toll taken by psoriasis can contribute to feelings of distress and diminished self-esteem. Therefore, an educated perspective on this condition helps in addressing not just the visible symptoms but also the underlying psychological effects.
Additionally, psoriasis is a complex interaction of genetic, environmental, and lifestyle factors. A comprehensive understanding of the condition prepares individuals to manage their symptoms more effectively and to navigate the challenges posed by flare situations.
This section serves as a foundational overview, enhancing awareness and understanding of the condition. Being informed about psoriasis allows both patients and practitioners to devise effective management strategies. This degree of insight can lead to improved quality of life for those living with the disorder. In essence, it empowers people to take informed steps toward alleviating symptoms and mitigating the psychological burdens associated with flare-ups.
Characteristics of Psoriasis Flare Symptoms
Understanding the characteristics of psoriasis flare symptoms is crucial for both individuals experiencing the condition and healthcare professionals. Recognizing these symptoms can foster early intervention and treatment, which ultimately reduces the severity and duration of flare-ups. This section aims to elucidate the physical and psychological symptoms associated with psoriasis, outlining how they manifest and their implications for quality of life.
Physical Symptoms
Patches of red skin
Red patches of skin represent a hallmark sign of psoriasis flares. This manifestation reflects inflammation and an overproduction of skin cells. Typically, these patches appear on the elbows, knees, and scalp, although they can emerge anywhere on the body. Their visibility significantly contributes to self-image concerns, as the affected individual may feel marked by the condition. While these patches are indicative of an active condition, one positive aspect is that they can be monitored for changes in patterns, signaling which treatments may need adjustment.
Scaly lesions
Scaly lesions often accompany the red patches. These lesions are areas where the skin becomes dry, thickened, and flaky. The characteristic scale is a result of the excess turnover of skin cells. While these lesions can be alarming, they serve an important role in identifying when a flare is in progress. Furthermore, scaly lesions can often symbolize ongoing inflammation, providing insights into the effectiveness of treatment regimens. Their presence reinforces the necessity for targeted management strategies.
Itching and burning sensations
The discomfort of itching and burning sensations adds another layer to the experience of psoriasis flare-ups. These sensations can range from mild to severe, and can often disrupt daily activities, resulting in increased stress levels. Recognizing itch intensity can inform treatment choices, guiding patients to recommended topical treatments that alleviate discomfort. \n\nThe pain associated with these sensations should not be overlooked, as it enhances the urgency for effective symptom management strategies.
Psychological Symptoms
Emotional distress
The emotional toll of experiencing psoriasis flares is profound. People with psoriasis often contend with feelings of frustration and helplessness due to the unpredictable nature of their condition. Emotional distress due to flare-ups can affect interpersonal relationships and daily activities, leading to a cyclical pattern of worsening flare severity. It is critical to acknowledge this element of psoriasis for a comprehensive approach to management, encompassing both physical and mental health.
Impact on self-esteem
Living with psoriasis can have a significant effect on self-esteem. The visible symptoms often lead to self-consciousness and social anxiety. The social stigma surrounding skin conditions can amplify feelings of inadequacy, affecting relationships and even career choices. Addressing self-esteem issues is vital for holistic care. Support systems, such as therapy or support groups, can offer a solution to mitigate the destructive impact of the condition on self-image.
Anxiety and depression
Anxiety and depression are common among individuals with psoriasis, particularly during flare periods. The chronic stress of managing a visible and unpredictable condition can trigger or exacerbate these mental health disorders. Ensuring that individuals receive mental health support alongside dermatological care is essential in creating a complete treatment protocol. Attending to both mental and physical health can improve overall well-being and quality of life for those affected.
"Understanding the full scope of psoriasis flare symptoms allows for a more tailored approach to management, ultimately benefiting individual quality of life."
Triggers of Psoriasis Flare-Ups
Understanding the triggers of psoriasis flare-ups is vital for effective management of the condition. By identifying and addressing these triggers, individuals can significantly reduce the frequency and severity of their symptoms. This part of the article examines various elements that contribute to flare-ups, tackling environmental, lifestyle, and genetic factors. Analyzing these triggers provides insights necessary for implementing preventative strategies that can enhance the quality of life for those affected.


Environmental Factors
Weather changes
Weather changes can have a notable impact on psoriasis flare-ups. Cold and dry conditions often lead to an increase in symptoms, making skin vulnerable to irritation. During the winter, the lack of humidity can cause skin to crack, exacerbating existing lesions. The unique feature of weather changes is how they can affect hydration levels in skin. This connection is crucial because maintaining moisture can mitigate flare-ups. Balancing indoor heating and the use of humidifiers can be beneficial in managing these effects.
Exposure to irritants
Exposure to irritants is another significant factor in triggering psoriasis flare-ups. Common irritants include harsh soaps, certain fabrics, and chemicals found in cleaning products. The key characteristic here is the direct harm these substances can cause, leading to increased inflammation in already sensitive skin. Individuals should consider opting for natural and hypoallergenic products as a way to minimize the risk of irritation. Avoiding known irritants can lead to fewer flare-ups and enhanced comfort in daily activities.
Infection risk
Infection risk poses a serious concern for psoriasis patients. Bacterial or viral infections can trigger or exacerbate flare-ups, leading to additional complications. The importance of understanding this risk is clear; preventing infections is crucial for maintaining stable skin conditions. Particularly, streptococcal infections have been linked to the onset of guttate psoriasis. This highlights the need for regular hygiene practices and prompt treatment of any infections to reduce flare-ups sensitively.
Lifestyle Choices
Stress management
Stress management is essential for those dealing with psoriasis. Psychological stress is known to trigger flare-ups, emphasizing the need for effective coping strategies. Meditation, deep breathing, and adequate sleep can be powerful tools in reducing stress levels. Their unique feature is that they not only help manage stress but can also improve overall well-being. A consistent stress management routine often leads to better skin health and fewer skin irritations.
Diet and nutrition
Diet and nutrition play a substantial role in managing psoriasis flare-ups. An anti-inflammatory diet rich in fruits, vegetables, and omega-3 fatty acids can be particularly beneficial. The key characteristic of this approach is the impact on the body’s inflammatory response. Prioritizing foods that fight inflammation can decrease the severity of flare-ups. However, it is essential to monitor personal reactions to specific foods, as some individuals may have unique triggers.
Substance use
Substance use is a critical lifestyle choice that can affect psoriasis symptoms. Alcohol and smoking have been linked to increased severity and frequency of flare-ups. The key aspect to recognize is that reducing or eliminating these substances can improve psoriasis outcomes. Unique to this discussion is the impact these substances have on the immune system, which can worsen the condition. In many cases, lifestyle changes that include reducing substance use lead to improved health and well-being.
Genetic Predisposition
Family medical history
Family medical history is an important consideration in understanding psoriasis flare-ups. Genetics can play a significant role in one’s susceptibility to this condition. Individuals with a family history of psoriasis may have inherited specific traits that increase their risk. Recognizing this connection can assist in early diagnosis and management approaches. Knowledge of family medical history allows for better-informed choices regarding lifestyle and treatment plans.
Associated genetic markers
Associated genetic markers are being researched for their contribution to psoriasis development. Certain genetic traits have been identified as risk factors for developing psoriasis. Understanding these markers can guide future strategies for prevention and treatment. Unique here is how genetic information can lead to targeted therapies. This emerging area of research is paving the way for advances in personalized medicine related to psoriasis management.
Diagnosing Psoriasis Flare Symptoms
Diagnosing psoriasis flare symptoms is a crucial aspect of managing the condition effectively. Recognizing the nuances of psoriasis is essential for ensuring proper treatment and care. Accurate diagnosis can lead to timely interventions, which can drastically improve the quality of life for individuals affected by this chronic skin disorder. Several methods of diagnosis exist, each contributing distinct advantages.
Clinical Evaluation
Clinical evaluation encompasses the assessment methods used by healthcare professionals to identify psoriasis flare symptoms. This evaluation is pivotal as it lays the foundation for further assessments and treatments.
Physical Examination
The physical examination is a direct method doctors use to observe and evaluate skin symptoms. In the context of psoriasis, it involves looking at patches on the skin to assess their appearance, distribution, and severity. This method is valued for its immediacy; it allows for quick identification of common indicators of flare-ups such as redness and scaling.
One key characteristic of the physical examination is its non-invasive nature. That means it can often be performed during a routine visit, making it accessible for many patients. The main advantage of this approach is that it provides immediate feedback to both patient and doctor about the condition. However, reliance solely on visual examination might overlook some underlying issues, such as systemic involvement.
Patient History
Patient history refers to the comprehensive review of an individual's past medical records alongside an interview about their symptoms. This step is vital for diagnosing psoriasis as it helps determine the duration and progression of symptoms, personal triggers, and family history of skin issues. This approach allows for a holistic understanding of the patient’s condition.
The strength of gathering patient history lies in its ability to contextualize current symptoms. By connecting past and present experiences, practitioners can better assess and anticipate future flare-ups. This method is particularly advantageous in identifying patterns that may not be visible during a physical examination. However, it relies significantly on accurate and honest reporting from the patient, which can sometimes pose challenges.
Laboratory Tests
Laboratory tests complement clinical evaluations by providing more definitive answers regarding a patient’s psoriasis. These tests can confirm a diagnosis and rule out other conditions that may present similarly.
Skin Biopsy
A skin biopsy involves taking a small sample of the affected skin for detailed examination under a microscope. This method can be crucial for individuals with atypical presentations of psoriasis, as it helps distinguish psoriasis from other skin disorders.
The key characteristic of a skin biopsy is its precision. It directly analyzes the skin structure, revealing alterations that are indicative of psoriasis. By providing definitive evidence, a biopsy can confirm the diagnosis with high accuracy. The disadvantage, however, is that it is an invasive procedure; some patients may feel discomfort or anxiety about undergoing such a test.
Blood Tests
Blood tests are another diagnostic tool in psoriasis management. These tests can help evaluate systemic inflammation and rule out other health issues contributing to skin symptoms. They may measure specific markers associated with psoriasis.
The primary benefit of blood tests lies in their ability to provide comprehensive insight into a patient’s overall health. They can uncover concurrent conditions, allowing healthcare providers to develop integrated treatment plans. However, while blood tests offer a broader perspective, results can sometimes lack the specificity needed for a clear-cut psoriasis diagnosis, relying instead on correlational data.
Proper diagnosis plays a pivotal role in managing psoriasis effectively. Without accurate assessment, treatment plans may miss the mark, leading to unnecessary suffering and complications.
Treatment Approaches for Psoriasis Flare Symptoms
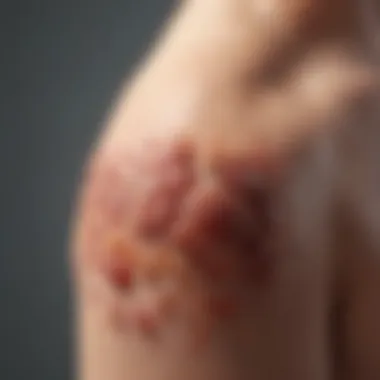

Treatment approaches for psoriasis flare symptoms are critical for managing this chronic condition effectively. The combination of different therapies is often necessary to combat both the physical and psychological symptoms that arise during flare-ups. Understanding the unique roles of topical, systemic, and phototherapy options allows patients to make informed choices conducive to their specific needs.
Topical Treatments
Topical treatments are frequently the first line of defense against psoriasis flare symptoms. They are applied directly to the skin, targeting localized areas of discomfort and irritation.
Corticosteroids
Corticosteroids are one of the most commonly used topical treatments because they help reduce inflammation and lower immune system response. They can lead to quick relief in red, inflamed patches associated with flare-ups. A key characteristic of corticosteroids is their varying strengths, allowing for tailored treatment plans. While they are effective due to their anti-inflammatory properties, extended use may result in skin thinning or other side effects. Therefore, it is important to use them under medical supervision to minimize risks.
Vitamin analogs
Vitamin D analogs are another essential category of topical treatments. They work by slowing down the rapid skin cell growth typical in psoriasis. A significant feature of these treatments is their ability to enhance the effectiveness of corticosteroids when used together. However, they may take longer to show noticeable results compared to corticosteroids. Potential side effects can include mild skin irritation, making dermatological guidance beneficial.
Moisturizers
Moisturizers represent a supportive element in treating psoriasis. They help reduce dryness and improve skin barrier function, which is often compromised in affected individuals. The key characteristic of moisturizers is their versatility and lack of adverse effects, making them suitable for daily use alongside other treatments. Although moisturizers do not address inflammation directly, they play a crucial role in alleviating symptoms and preventing flare-up triggers.
Systemic Treatments
Systemic treatments are essential for managing more severe or widespread cases of psoriasis. These treatments affect the entire body rather than just localized areas, thus providing comprehensive management options.
Biologic therapies
Biologic therapies are an innovative advancement in treating psoriasis, targeting specific parts of the immune system. They are particularly useful for moderate-to-severe cases where traditional therapies are ineffective. A key feature is their targeted action, which minimizes systemic side effects. Biologics are a popular choice due to their potential for long-term control of the condition. However, they often require close monitoring because of potential immunosuppression and the need for injection or infusion.
Oral medications
Oral medications, such as methotrexate or acitretin, play a vital role in systemic therapy. They can effectively reduce inflammation and improve psoriatic conditions. A notable characteristic is their convenience, as they do not require application to the skin. However, the use of oral medications may lead to side effects, including gastrointestinal issues and liver toxicity. Regular follow-up and laboratory assessments are essential to monitor their effects.
Phototherapy Options
Phototherapy options provide a non-invasive alternative for treating psoriasis flare symptoms through controlled exposure to ultraviolet light.
UVB therapy
UVB therapy is a widely utilized phototherapeutic approach, effective in treating psoriasis by slowing down skin cell turnover. A significant feature of UVB therapy is its ability to target affected areas while minimizing damage to surrounding skin. Its role in reducing flare intensity is clear, but patients must adhere to treatment schedules to experience benefits consistently. Side effects can include skin damage if exposure is not properly monitored.
PUVA therapy
PUVA therapy combines a photosensitizing drug with UVA light exposure. It can offer significant relief for patients with resistant psoriasis. The key characteristic of PUVA therapy is its ability to penetrate deeper layers of skin, providing effective treatment for stubborn lesions. Despite its effectiveness, PUVA carries risks such as increased chances of skin cancer and requires rigorous precaution measures. Patients should consult with healthcare providers to assess suitability and safety.
In summary, understanding treatment approaches for psoriasis flare symptoms allows individuals to explore various options tailored to their condition. This knowledge helps facilitate productive discussions with healthcare providers, ensuring that each step taken towards managing this challenging disease is well-informed.
Lifestyle Modifications to Manage Flare Symptoms
Managing psoriasis flare symptoms involves understanding various lifestyle changes that can help reduce severity and frequency of outbreaks. Lifestyle modifications offer a proactive approach that empowers individuals to take charge of their health. Incorporating these adjustments not only enhances quality of life but also contributes to overall symptom management. It is essential to consider individual preferences and needs when implementing these changes.
Nutritional Adjustments
Anti-inflammatory diet
An anti-inflammatory diet focuses on reducing inflammation in the body, which is particularly relevant for individuals suffering from psoriasis. This dietary approach emphasizes the consumption of whole foods such as fruits, vegetables, whole grains, and healthy fats like those found in olive oil and fatty fish.
The key characteristic of this diet is its emphasis on natural foods while minimizing processed options that can exacerbate inflammation. Adopting this dietary pattern can lead to benefits like reduced flare severity and better overall health. However, it may require guidance from a healthcare professional to ensure nutritional balance and effectiveness.
A unique feature of the anti-inflammatory diet is its flexibility, allowing individuals to adapt their food choices based on taste while adhering to health goals. One potential disadvantage might be the challenge of maintaining such a diet, especially in social settings where processed foods are prominent.
Hydration practices
Hydration plays a crucial role in skin health and overall wellbeing. Proper hydration helps maintain skin elasticity and can reduce the intensity of psoriasis flare symptoms. The key characteristic of hydration practices is their simplicity; it primarily involves drinking adequate water throughout the day.
These practices are beneficial because they promote internal health while potentially minimizing dryness and irritation of the skin common in psoriasis.
A unique feature of hydration is its accessibility; water is readily available and free for most. However, individuals may find it difficult to remember to drink enough water daily, particularly if they have busy schedules.
Stress Reduction Techniques
Meditation and mindfulness
Meditation and mindfulness are effective techniques that can significantly influence the management of psoriasis flare symptoms. These practices focus on improving mental clarity and emotional regulation, which can reduce stress—one of the notable triggers for psoriasis. The fundamental characteristic of these techniques is their ability to promote a state of relaxation and awareness.
Engaging in regular meditation can lead to benefits like enhanced emotional resilience and better coping strategies concerning flare symptoms. Nonetheless, mastering these techniques can take time and effort, and consistency is key.
A unique feature of these practices is their inclusivity, as anyone can implement them regardless of experience level. However, some individuals may find it challenging to maintain focus during initial attempts.
Physical activity
Physical activity is another vital component for managing psoriasis flare symptoms. Engaging in regular exercise can improve circulation, enhance mood, and even boost immune function. The key characteristic of physical activity is its numerous forms, ranging from walking to structured workouts.
This is a popular choice as it not only reduces stress but also promotes physical health and improves overall wellbeing.
A unique feature of physical activity is its adaptability; individuals can choose the intensity and type of exercise that suits their preferences. Some disadvantages may include difficulty in sticking to a routine or potential physical limitations depending on individual health status.
Skin Care Regimens


Regular moisturizing
Regular moisturizing is essential for those managing psoriasis. Keeping skin hydrated can minimize the dryness and itching commonly associated with flare-ups. The fundamental characteristic of this practice is its emphasis on daily application of appropriate moisturizers to maintain skin hydration.
This practice is beneficial as it creates a protective barrier on the skin, promoting healing and comfort. However, it can require discipline to make it a consistent part of daily routine.
A unique feature of regular moisturizing is the range of products available, from lotions to ointments, allowing personalization based on skin type. But individuals may find it overwhelming to choose among various options, leading to potential ineffectiveness if the wrong products are selected.
Avoiding skin irritants
Avoiding skin irritants is crucial for managing psoriasis flare symptoms. It involves recognizing and steering clear of substances that can cause skin reactions. The key characteristic of this approach is its preventive nature, enabling individuals to take control of potential flare triggers.
This choice is beneficial as it can significantly reduce the incidence and severity of outbreaks when incorporated into daily life.
A unique feature of this strategy is its reliance on individual observation and adjustment; what irritates one person may not cause issues for another. However, the downside can involve a learning curve to identify all potential irritants effectively.
Potential Complications of Psoriasis
Understanding the potential complications of psoriasis is essential for managing this condition effectively. The impact of psoriasis extends beyond the skin, affecting various aspects of life including physical health and mental well-being. Identifying these complications can facilitate early intervention, improving patient outcomes.
Joint Issues
Psoriatic arthritis
Psoriatic arthritis is a significant complication associated with psoriasis. It manifests as a painful, inflammatory joint disease that can develop in individuals who already have psoriasis. This connection underscores the importance of monitoring joint health in psoriasis patients. The key characteristic of psoriatic arthritis is the inflammation it causes, which can lead to joint damage if not addressed timely.
The unique feature of psoriatic arthritis is its ability to present without prior joint complaints. This adds a layer of complexity to the diagnosis, making awareness of symptoms crucial for early detection. Notably, the advantage of recognizing this condition early allows for proactive management strategies, which can drastically improve the quality of life for the patient.
Mobility challenges
Mobility challenges arise as a direct consequence of joint issues caused by psoriatic arthritis. These challenges can lead to difficulties in performing daily activities, significantly impacting an individual's independence and overall quality of life. The key characteristic of mobility challenges is the restricted range of motion and pain during movement. This limitation can be frustrating and disheartening for individuals affected by it.
What sets mobility challenges apart is their ability to escalate if left unaddressed. Having a proactive approach to joint care can help mitigate these challenges. However, it’s essential to understand that while treatments exist, they may not fully restore function in advanced cases.
Psychological Impacts
Chronic sadness
Chronic sadness is a psychological impact that often accompanies psoriasis and its physical manifestations. Individuals may experience feelings of hopelessness and decreased motivation, which can deepen the struggle with their skin condition. This facet of psoriasis is vital to include because it emphasizes the intertwined relationship between physical and mental health. Chronic sadness can amplify the perceived severity of symptoms, making management more complex.
The unique feature of chronic sadness is its persistence; it doesn’t just arise during flare-ups but can become a chronic state. It's important to note that this psychological toll can hinder the efforts to manage psoriasis effectively, making it crucial to address mental health alongside physical symptoms.
Social isolation
Social isolation is another critical psychological impact of psoriasis that warrants attention. Many individuals with psoriasis find themselves withdrawing from social interactions due to embarrassment about their appearance. The key characteristic of social isolation is the avoidance of social situations, which can perpetuate a cycle of loneliness and negative mental health outcomes.
This aspect is particularly relevant as it highlights the societal stigma surrounding visible skin conditions. The unique feature of social isolation lies in its dual nature; it can be both a consequence of the disease and a contributing factor to its severity. Addressing social isolation through supportive networks and community engagement can bolster self-esteem and improve overall mental health.
Blockquote: Recognizing the complexities of psoriasis involves understanding both its physical symptoms and the potential psychological impacts, which play a crucial role in the overall experience of individuals living with the condition.
Future Perspectives on Psoriasis Management
Understanding the future perspectives on psoriasis management is vital for both patients and healthcare professionals. The landscape of treatment is evolving rapidly, driven by advances in research and technology. Patients benefit from this progression as emerging therapies and personalized approaches promise to enhance treatment efficacy.
Moreover, ongoing research into the underlying causes of psoriasis paves the way for better management strategies. These advancements signify hope for more targeted and effective interventions that can improve patients' quality of life.
Advancements in Therapies
Emerging drug treatments
Emerging drug treatments represent a significant leap in psoriasis management. These innovative drugs aim to target specific pathways involved in the inflammatory processes of psoriasis. By focusing on particular immune responses, these treatments offer more tailored interventions. A key aspect of these drugs is their ability to reduce flare-ups while minimizing side effects.
The unique feature of emerging drug treatments is their designed precision. Unlike traditional treatments that might affect the entire immune system, these new medications often concentrate on specific cells or cytokines. This specificity can lead to better outcomes, but it may also come with high costs and the necessity for careful monitoring.
Personalized medicine
Personalized medicine is reshaping the approach to treating psoriasis. This method tailors treatments based on individual genetic makeup and response to therapies. It allows for a more accurate selection of treatment options. This way, healthcare providers can identify which therapies are more likely to succeed for each patient.
A key characteristic of personalized medicine is the focus on individual variability. This approach can significantly enhance treatment effectiveness. However, personalized treatment can also be complex and may require broader access to genetic testing and advanced diagnostics.
Research on Underlying Causes
Genetic research
Genetic research is uncovering the complex genetic factors influencing psoriasis. This area of study has provided insights into how certain genes predispose individuals to this skin condition. By understanding genetic markers, researchers can develop better-targeted treatments.
A notable advantage of this research is the potential to predict disease severity and treatment responses. However, genetic research can be costly and time-consuming, presenting challenges in implementation across diverse populations.
Immune system studies
Immune system studies offer crucial insights into how psoriasis affects the body's defense mechanisms. Research focusing on immune responses is shedding light on how psoriasis flares can be managed more effectively. By studying immune pathways, scientists hope to develop targeted therapies that directly address these mechanisms.
A significant benefit of immune system research is its potential to reveal new therapeutic targets. However, studying the immune system is inherently complex, and translating findings into practical treatments may take time.
The future of psoriasis management holds great promise, combining innovative therapies with personalized approaches to improve outcomes.
In summary, the future directions in psoriasis management focus on advancements in therapies and a deeper understanding of genetic and immune factors. As research progresses, the landscape of treatment options is likely to expand, offering new hope to those living with psoriasis.







