Advancements in Clinical Trials for Artificial Kidneys


Intro
The exploration of artificial kidneys stems from the relentless advancement in medical technology, particularly in organ replacement therapies. The urgency to develop these devices is primarily driven by the staggering statistics of kidney disease. Millions suffer from chronic kidney conditions, necessitating dialysis or transplantation. Amid the quest for innovative solutions, clinical trials emerge as vital stepping stones. They provide a structured methodology to evaluate the safety and efficacy of artificial kidneys, fostering trust and understanding among both the scientific community and potential patients.
As this article progresses, we will delve into the intricacies of clinical trials related to artificial kidneys. This will cover their phases, methodologies, as well as the ethical frameworks that govern them. A closer look at participant engagement and regulatory challenges offers a comprehensive understanding of the landscape. Furthermore, we will highlight the potential ramifications of these trials on the future of patient care and healthcare systems at large.
Foreword to Artificial Kidneys
Defining Artificial Kidneys
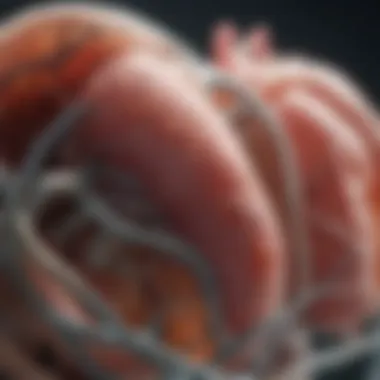
Artificial kidneys, also known as bioartificial kidneys or renal replacement therapies, refer to devices designed to replicate the kidney's essential functions. These functions include the filtration of blood to remove waste products, balancing electrolytes, and maintaining fluid levels in the body. Unlike traditional dialysis, which merely performs a filtering function, advancements aim to create devices that more closely mimic the biological processes of a natural kidney.
Artificial kidneys can be classified into two main types: external and implantable devices. External devices, like wearable artificial kidneys, are still in experimental stages, while implantable devices often involve bioengineering techniques that integrate living renal cells with bio-compatible materials. This synergistic approach is crucial for improving patient outcomes and quality of life in individuals with kidney failure.
Historical Context and Development
The journey toward developing artificial kidneys began in the mid-20th century, marked by the invention of the first dialysis machine by Dr. Willem Kolff. The initial use of these devices provided life-saving treatment for patients suffering from kidney failure. Since then, substantial progress has been made. Research efforts have evolved from simple mechanical filtration to complex systems that employ cellular biology and engineering.
In the 1990s and early 2000s, advancements focused on improving biocompatibility and reducing the complications associated with long-term dialysis. The introduction of bioartificial kidneys, which began incorporating living cells, has opened new avenues for research. Current trials aim to assess various configurations and applications of these devices to ensure optimal performance when deployed in clinical settings.
As the necessity for effective kidney replacement solutions grows, understanding the foundational aspects of artificial kidneys sets the stage for a detailed exploration into the corresponding clinical trials. The examination of trials will elucidate the necessary scientific rigor involved in confirming the viability of these groundbreaking advancements, shaping the future of renal care.
The Importance of Clinical Trials
Clinical trials are foundational to developing medical innovations, especially for complex areas like artificial kidneys. They serve as a systematic approach to testing theories, assessing effectiveness, and ensuring safety before new treatments can be available to the public. These trials create a structured environment for researchers to gather data that inform healthcare providers and patients about the potential benefits and risks associated with a new treatment.
One crucial element of clinical trials is their role in demonstrating the efficacy of artificial kidney technologies. By rigorously testing these solutions through clinical studies, researchers can identify how well they function in real-world scenarios. This not only enhances the credibility of the technology but also assures healthcare practitioners and patients of its benefits.
Additionally, clinical trials contribute significantly to the innovation process. They provide a platform for novel ideas to be rigorously evaluated, allowing for iterative improvements. For instance, if certain designs for an artificial kidney perform poorly in initial phases, researchers can refine their approach based on collected data. The ability to adapt and change strategies based on solid evidence is essential for advancing medical technology.
Moreover, clinical trials play a vital role in establishing guidelines and best practices in the medical field. They help to define standards of care that can be widely adopted by practitioners. Following successful trials, outcomes and findings are often published, contributing to the body of knowledge in nephrology and renal care. These publications can guide clinicians in their decision-making processes, which ultimately enhances patient care.
In summary, the importance of clinical trials cannot be overstated. They are integral to ensuring that artificial kidneys are safe and effective before they reach market. The iterative nature of trials fosters innovation while simultaneously grounding medical practice in tested science. As such, they create a bridge between theoretical research and practical application.
Role in Medical Innovation
Clinical trials are a driving force behind medical innovation. They provide an essential pathway for new therapies and technologies to receive validation. In the case of artificial kidneys, trials reveal critical information regarding their functionality and patient outcomes. This process not only assesses the immediate benefits but also collects long-term data regarding health impacts and quality of life for kidney-related ailments.
Conducting a well-structured clinical trial requires collaboration among numerous stakeholders including researchers, medical professionals, and regulatory bodies. This collaboration is pivotal for innovations to transition from concept to clinical practice. Successful trials can lead to breakthroughs that carve pathways for similar life-saving innovations in nephrology and beyond.
Ethical Considerations in Trials
Ethics is a cornerstone of clinical trials. When investigating new treatments for artificial kidneys, it is crucial to prioritize participant safety and informed consent. Participants should have a clear understanding of the trial’s purpose, what procedures will entail, and any potential risks involved. The informed consent process must be transparent, ensuring that patients make educated choices about their involvement.
Furthermore, ethical oversight is provided by institutional review boards. These boards evaluate trial protocols to ensure that they meet ethical standards and protect the health and welfare of participants. Ethical frameworks require ongoing monitoring of trials to safeguard against adverse effects and ensure modifications are made if needed.
Another ethical concern is equity in access to trials. It is essential to ensure diverse participant representation, reflecting varied demographics and backgrounds. Inclusive recruitment practices can lead to more comprehensive data, promoting fairness in medical advancements.
Phases of Clinical Trials
Phase One: Safety and Dosage
In the first phase of clinical trials, the primary focus is on safety. Researchers administer the artificial kidney to a small group of healthy volunteers or patients. This phase aims to determine the appropriate dosage and assess any immediate adverse effects. Measurements such as renal function, blood pressure, and biochemical markers are closely monitored.
The importance of this phase cannot be overstated; safety is paramount in any medical intervention. Researchers gather data on how the body responds to the artificial kidney. This information helps them identify any potential risks associated with the technology. Furthermore, understanding dosage informs future phases of the trial, laying the groundwork for further efficacy testing.


"Safety is not an option; it’s a foundation upon which all further developments are built."
Phase Two: Efficacy and Side Effects
Phase two trials are critical for evaluating the efficacy of the artificial kidney. In this stage, researchers involve a larger group of participants suffering from kidney diseases. The aim is to understand whether the device functions as intended and how it affects the patient’s condition. Data collected includes indicators like kidney function improvements, biochemical adjustments, and overall patient well-being.
Additionally, this phase focuses on identifying side effects. While some adverse effects might have surfaced in phase one, phase two provides a more extensive view of any complications. This knowledge is vital in refining the technology and improving patient outcomes. Evaluating both efficacy and safety creates a balanced perspective for clinicians and stakeholders.
Phase Three: Comparison to Standard Treatments
The third phase is crucial as it compares the artificial kidney to existing standard treatments, such as dialysis or transplantation solutions. During this phase, large-scale trials are conducted, often involving multiple centers. The goal is to assess whether the artificial kidney provides superior outcomes.
Researchers focus on metrics such as recovery time, quality of life, and long-term health benefits. This phase can be time-consuming, but it establishes statistical evidence that can influence regulatory approvals. Results from this phase will determine if the artificial kidney can reach the market and how it will be positioned within the current treatment landscape.
Phase Four: Post-Market Surveillance
Once an artificial kidney receives approval, it enters phase four, known as post-market surveillance. Even after a clinical trial has established safety and efficacy, ongoing monitoring is essential. This phase ensures continued assessment of the device's performance in real-world settings.
Healthcare providers collect data on long-term outcomes, unexpected side effects, and overall patient satisfaction. This information feeds back into the research, providing insights that can lead to enhancements in future iterations of the technology. Surveillance ensures that the artificial kidney remains beneficial and maintains a high safety profile once used widely in the healthcare system.
Research Methodologies in Trials
Research methodologies form the backbone of clinical trials, guiding how studies are designed and implemented. These methodologies are crucial for ensuring that the data collected is reliable and valid, ultimately influencing the trial's outcomes. In the context of artificial kidney research, methodologies help address specific objectives, such as assessing the effectiveness and safety of these innovative treatments. Recognizing the significance of these methodologies can lead to better study designs and more meaningful results.
Randomized Control Trials
Randomized control trials (RCTs) are considered the gold standard in clinical research due to their robust design. In an RCT, participants are randomly assigned to either the treatment group receiving the artificial kidney or a control group receiving standard care. This method minimizes bias, ensuring that any observed effects can be confidently attributed to the treatment itself rather than external factors. RCTs provide crucial evidence on efficacy and safety, which is particularly important for novel technologies like artificial kidneys.
The process of randomization helps create similar groups, balancing known and unknown confounding variables. This balance enhances the internal validity of the trial. Some key considerations include:
- Ensuring sample size is adequate for statistical power.
- Establishing clear inclusion and exclusion criteria to ensure relevant participant selection.
- Maintaining blinding where possible to reduce bias in outcomes.
"Well-designed randomized control trials are essential for determining the true benefit of artificial kidney technologies."
Observational Studies
There are several types of observational studies, including cohort studies, case-control studies, and cross-sectional studies. Each type serves different research purposes with its own strengths and weaknesses.
Key aspects of observational studies:
- They can be conducted relatively quickly and at lower costs compared to RCTs.
- They allow for a broader range of data collection, including adverse effects that may occur over time.
- Potential biases, such as selection bias and confounding, must be carefully considered when interpreting results.
Together, RCTs and observational studies provide a comprehensive approach to understanding the impact and effectiveness of artificial kidney technologies, guiding future innovations in the field.
Challenges in Conducting Clinical Trials
Recruitment of Participants
Recruiting participants for clinical trials is fundamental. The success of a trial often hinges on the ability to attract the right demographics. Patient eligibility criteria can be strict, which narrows the pool of potential candidates. Many patients face health complications that may make them ineligible. In some cases, patients may be hesitant to join due to fear of side effects or uncertainty about new treatments.
Effective recruitment strategies must consider these challenges. Engagement with healthcare professionals is crucial. When doctors understand the benefits of the trial, they can encourage eligible patients to participate. Furthermore, public awareness campaigns can help demystify clinical trials and reduce stigma or fear around experimental treatments. Successful recruitment can yield a more diverse participant base, ultimately leading to more generalized and applicable results.
Funding and Resources
Funding is another critical challenge. Clinical trials require significant financial investment for everything from personnel to technology. The development of artificial kidneys, specifically, demands resources for sophisticated equipment and comprehensive patient monitoring. Securing funding can be difficult. Many researchers rely on grants or partnerships with pharmaceutical companies, and competition for these funds is intense.

A lack of funding can lead to compromised study designs or insufficient participant enrollment, influencing the reliability of results. Therefore, establishing partnerships with biotechnology firms or seeking government funding can be vital. Moreover, clear communication about the potential impact of artificial kidney technology can attract interest from investors or stakeholders concerned with healthcare innovation.
Regulatory Hurdles
Navigating regulatory hurdles presents another layer of complexity. Regulatory agencies like the FDA and EMA impose stringent guidelines to ensure patient safety and data integrity. While these regulations are essential, they can slow down the pace of clinical trials. The approval process for trial protocols often involves extensive documentation and multiple reviews, which can be time-consuming.
Researchers must be diligent in understanding the requirements set forth by regulatory bodies. Early engagement with these agencies can make a significant difference. Clarity about trial design and methodology not only aids in compliance but fosters transparency. This proactive approach may contribute to smoother approvals and faster progress in artificial kidney development.
Overall, tackling the challenges associated with conducting clinical trials requires a multifaceted strategy. From enhancing participant recruitment techniques to securing financial backing and navigating regulations, successful clinical trials demand careful planning and collaboration.
Regulatory Framework for Trials
The regulatory framework governing clinical trials is a critical aspect for the development of artificial kidneys. It ensures that the trials are conducted in a safe, ethical, and scientifically sound manner. This framework not only establishes the safety and efficacy of new treatments but also protects the rights and well-being of participants involved in these trials.
The importance of the regulatory framework can be seen in various elements. Firstly, it provides guidelines for trial design, which dictate how studies should be structured to yield reliable results. Secondly, it outlines the approval process for new technologies such as artificial kidneys, necessitating comprehensive data collection and evaluation before a product can be deemed safe for public use. This creates a balance between rapid innovation and necessary scrutiny.
Additionally, this framework promotes transparency in trial conduct. Researchers are required to register their studies and publicly disclose results, fostering an environment of trust and collaboration within the scientific community.
Roles of the FDA and EMA
Similarly, the EMA implements legislation in European contexts that aligns with the evolving needs of medical research. By harmonizing regulations across member states, the EMA facilitates not only approval processes but also post-market surveillance. This vigilant oversight helps mitigate risks associated with new technology, allowing for a pathway to quick resolution should any complications arise.
Regulatory bodies serve as gatekeepers, ensuring the integrity of clinical trials and the safety of participants.
International Standards and Guidelines
International standards and guidelines play a fundamental role in the consistency of clinical trials across different regions. Organizations such as the World Health Organization and the International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use set forth principles that ensure the quality and ethical conduct of trials globally.
These standards encompass Good Clinical Practice (GCP), which mandates adherence to ethical and scientific quality in designing, conducting, and reporting clinical research. By following these international guidelines, stakeholders can compare results from trials conducted in various countries, ultimately fostering a collaborative atmosphere that promotes faster advancements in technology.
Moreover, by aligning research practices with these standards, researchers enhance the credibility of their findings, thus supporting the acceptance of data among regulatory bodies and the global medical community.
Patient Engagement in Clinical Trials
Patient engagement in clinical trials is essential for the advancement of artificial kidney research. Engaged patients provide meaningful contributions to the design, implementation, and outcomes of trials. Their perspectives help refine research objectives and ensure that the trials address real-world needs. By fostering engagement, researchers can improve participant retention and the quality of data collected.
Informed Consent Process
The informed consent process is a fundamental aspect of patient engagement in clinical trials. It ensures that participants understand the nature of the trial, including potential risks and benefits. During this process, researchers must clearly communicate information in a way that is accessible to varying levels of health literacy.
Patients should be encouraged to ask questions and express concerns. This dialogue not only builds trust but also allows researchers to address any misunderstandings. It is vital that participants feel fully informed before they agree to take part in a trial, as it empowers them and respects their autonomy. This process can be enhanced through tools like visual aids and simplified language pamphlets, making the information more relatable and easier to digest.
Patient Education and Awareness
Patient education and awareness play a crucial role in facilitating engagement in clinical trials. Educated patients are more likely to participate and adhere to trial protocols. There are several strategies that can promote effective education:
- Workshops and Seminars: Organizing events to inform potential participants about the trials and the artificial kidneys’ technology.
- Online Resources: Providing accessible content on websites or forums helps patients learn at their own pace. Resources could include articles, videos, and FAQs.
- Support Networks: Fostering communities where patients can connect and share their experiences can enhance understanding and reduce anxiety.
These educational efforts can demystify the clinical trial process and foster a culture of participation. When patients feel informed and involved, the overall success of clinical trials is likely to improve, leading to faster advancements in artificial kidney technology.
Key Clinical Trials in Artificial Kidney Research
Clinical trials are vital in the quest to develop an effective artificial kidney. They help in understanding how such devices can operate safely and efficiently within the human body. With populations suffering from kidney disease steadily increasing, the urgency for innovative solutions has risen. Artificial kidneys could potentially minimize the burden on transplant lists and offer enhanced quality of life for patients. This section explores notable clinical trials and the significant findings that emerged from them, as well as provides a comparative analysis of the results from these trials.
Notable Trials and Findings

One landmark trial is the FREEDOM study, which evaluated the performance of the Wearable Artificial Kidney (WAK). Participants wore a device that continuously removes toxins and excess fluid, mimicking natural kidney function. Preliminary results suggested that patients experienced improved fluid management and reduced hospital visits compared to traditional dialysis methods.
Another essential trial is the study on the Kidney Project's bioartificial kidney. This device combines a hemofilter with living renal cells. Initial findings indicate successful biocompatibility with human tissues, leading to better patient outcomes. This exciting advancement demonstrates promise for providing kidney function without the need for external machines.
Additionally, the Biodesign trial focused on the long-term impact of implantable devices on heart and kidney health. The aim was to assess overall morbidity and quality of life in patients. Participants reported a significant reduction in symptoms associated with kidney failure and an improved overall sense of well-being.
Comparative Analysis of Results
Comparing results from these trials is crucial for understanding the progress in artificial kidney research. The FREEDOM study's results highlighted significant advantages in fluid control over standard dialysis therapies, indicating a shift in how kidney treatment could evolve. The WAK showcased potential for improved patient autonomy, aligning with modern patient-centered care trends.
On the other hand, the Kidney Project's bioartificial kidney trial contributed a unique perspective by using living cells. This trial's outcomes emphasized biological interactions instead of mechanical solutions. The comparative benefits suggest a dual approach in artificial kidney design may be necessary, integrating both mechanical and biological components for optimal results.
"The future of renal care could hinge on these innovative trial outcomes, potentially reshaping treatment paradigms for chronic kidney disease."
In summary, these notable trials offer valuable insights into artificial kidney research. They not only highlight different methodologies but also the potential impacts on patient care and healthcare systems. As research progresses, comparative analyses from various trials will inform future approaches, paving the way for more comprehensive solutions to the challenges posed by kidney disease.
Future Directions in Artificial Kidney Development
The development of artificial kidneys stands at a critical juncture in medical science. As the burden of kidney diseases continues to rise, the need for efficient, reliable, and effective treatment options has never been more pressing. Future directions in this field not only promise advancements in technology but also aim to transform the way patients receive care. This section explores both the technological innovations driving this progress and the anticipated impact on patient care.
Technological Innovations
Emerging technologies are playing a significant role in the evolution of artificial kidneys. One of the most promising areas is the integration of bioengineering techniques. Researchers are exploring ways to create bioartificial kidneys that combine living kidney cells with synthetic materials. This may enhance the body's acceptance of the device and improve function.
Another avenue of exploration is the development of wearable dialysis devices. These devices aim to provide continuous monitoring and real-time adjustments in treatment, thus promoting better management of kidney diseases. For instance, innovations like portable hemodialysis units allow patients to receive treatment in comfort, reducing the need for frequent hospital visits.
Furthermore, advances in nanotechnology hold promise for building more efficient filtration mechanisms. Researchers believe that using nanoscale devices could mimic kidney functions more closely than traditional methods, potentially reducing complications associated with current dialysis treatments.
"The integration of these technologies could redefine patient outcomes and expectations in kidney care."
The role of artificial intelligence cannot be overlooked. By employing machine learning algorithms, healthcare providers can analyze vast data sets from clinical trials to predict outcomes and personalize treatment plans for patients on artificial kidney therapies.
Potential Impact on Patient Care
The potential impact of artificial kidneys on patient care is profound. An improved artificial kidney can reduce the need for conventional dialysis, thereby improving patient quality of life. The anxiety and social stigma often associated with regular treatments would diminish, allowing patients to lead more normal lives.
Additionally, the ability for these devices to operate continuously means that patients may experience fewer dietary restrictions. With real-time monitoring and adjustments, the dependency on strict dietary guidelines could be lessened, enabling patients to experience greater freedom.
The focus on personalized medicine through artificial kidney technology could enhance patient engagement. By leveraging data from devices, healthcare professionals can tailor treatments to meet individual needs. This could lead to more effective management of existing conditions, thereby improving overall health outcomes.
In summary, the future directions in artificial kidney development not only focus on technological enhancements but also aim to elevate patient care standards. This intersection of innovation and empathy is essential to advancing renal treatment and combating the growing challenges presented by kidney diseases.
Ending
The conclusion of this article serves to underscore the critical nature of clinical trials in the context of artificial kidney development. Clinical trials represent a fundamental step in transforming theoretical advancements into practical medical solutions. They provide evidence necessary for the safe and effective implementation of artificial kidneys, ultimately influencing patient outcomes.
Summary of Key Points
In summarizing the key points:
- Clinical trials are essential for testing the safety and efficacy of artificial kidneys.
- The trials go through multiple phases, each with specific goals and assessments.
- Methodologies such as randomized controlled trials and observational studies are crucial for generating reliable data.
- Challenges like participant recruitment and regulatory compliance pose significant hurdles.
- Patient engagement is vital for gathering diverse perspectives that influence trial results.
By capturing these elements in the summary, we can see the multifaceted approach necessary in addressing the complexity of artificial kidney research. This collective knowledge contributes to a greater understanding of the potential benefits and risks associated with this innovative technology.
Implications for Healthcare Systems
The implications of advancing artificial kidney technology are profound for healthcare systems worldwide. As these devices move from experimental trials to clinical use, they have the potential to:
- Alleviate kidney disease prevalence: With improved access to artificial kidneys, we can expect a reduction in the burden on transplant lists.
- Enhance patient care: These technologies can lead to better management of kidney-related complications, improving overall quality of life for patients.
- Shift healthcare resources: The integration of artificial kidneys may streamline resources, allowing for more efficient use within healthcare systems.
As healthcare professionals, researchers, and policymakers consider these advances, the dialogue must continue. Collaborative efforts across disciplines will be key to maximizing the positive impacts on public health and ensuring equitable access to life-saving technologies.







